Highlights
- As on June 30, Uttar Pradesh had 6,650 active COVID-19 cases
- Uttar Pradesh has dedicated 135 hospitals for treatment of COVID-19
- The state is testing over 20,000 people per day: UP Government
New Delhi: Uttar Pradesh (UP) with more than 20 crore residents, as per the Population Census 2011, is the most populous state in the country. In fact, the size of the population of UP is equivalent to the European Union’s three major countries- Germany, the United Kingdom, France combined. Out of the total, the population of the state 77.7 per cent live in rural areas and according to the Ministry of Social Justice and Empowerment, about one-third of the population of the state live below poverty line (BPL) which means that about 1in 3 persons are living on an income of Rs. 356 per month in rural areas and Rs. 538 per month in urban areas. According to experts, the high level of poverty and high density of population, with 828 people per square kilometre, make the state vulnerable in the situation of medical crisis such as the ongoing COVID-19 pandemic.
Also Read: COVID-19: Uttar Pradesh Chief Minister Instructs To Form 1 Lakh Teams For Effective Surveillance
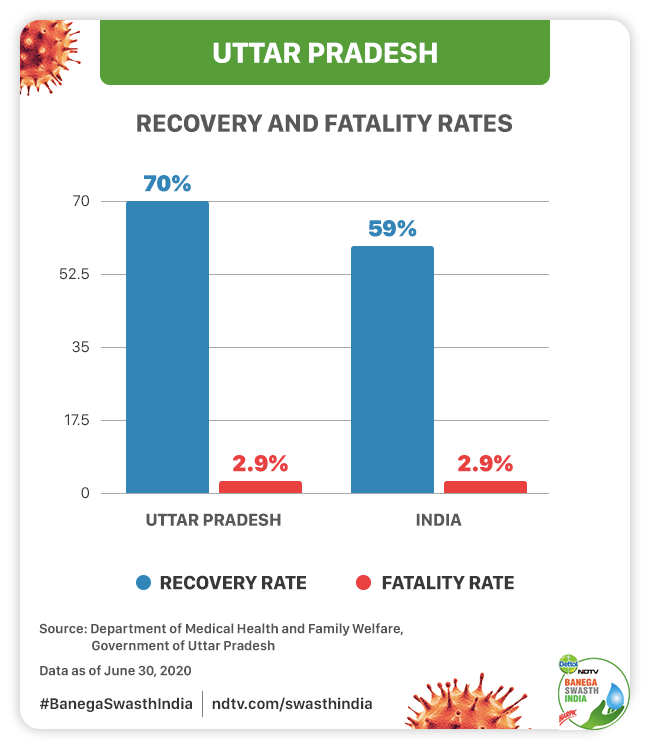
Currently, UP is the fifth worst-affected state of the country. The state claims to have a recovery rate of about 70 per cent which is higher as compared to the national average of 59 per cent, as on June 30. However, keeping the mortality rate low is what the state is striving to overcome which is currently 2.9 per cent at par with the national average of 2.9 per cent.
Here is how the state is fighting the challenges of COVID-19 pandemic.
Big Jump In Cases In May, High Number Of Cases And Deaths In Western Districts A Big Worry
The first case of the COVID-19 pandemic in Uttar Pradesh was reported on March 4 in Ghaziabad when a middle-aged man who had a travel history to Iran was tested positive. By the end of March, the number of cases in UP crossed 100. In April, the number of cases in the state started doubling every three days, despite the lockdown, which as per the experts maybe because of the infections caught before the lockdown was imposed. The doubling rate improved to 16 days by the end of the second lockdown. However, the number of cases started increasing progressively and by the end of May, there were 7,445 confirmed cases of COVID-19 in the state. According to Amit Mohan Prasad, Principal Secretary (Health), the spike in the number of cases can be attributed to return of migrant workers and increase in testing per day from only 100 in March to over 10,000 per day in May.
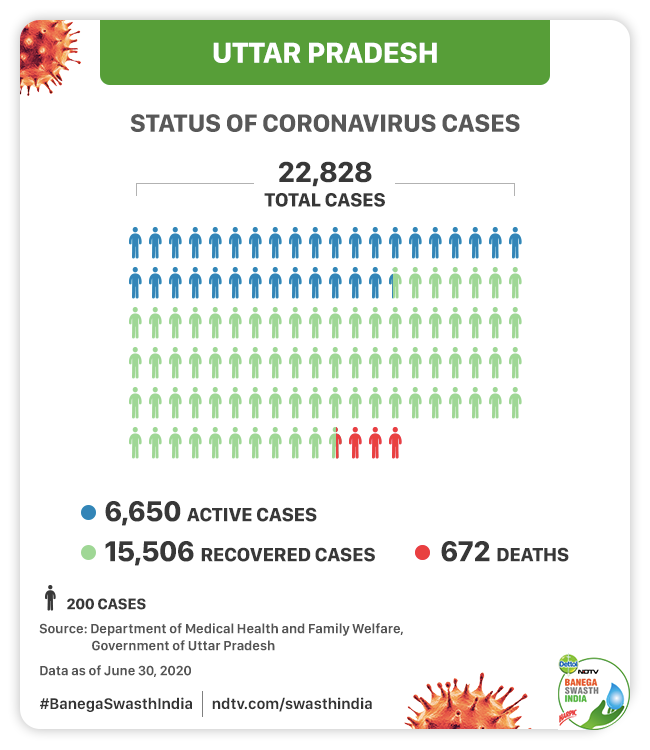
As of June 30, Uttar Pradesh has reported a total of 22,828 positive cases, including 6,650 active cases. The total fatalities as on June 30 are 672 deaths. The state has been able to cure 15,506, according to the data reported by the Department of Medical Health and Family Welfare of Uttar Pradesh.
Over 70 per cent of COVID-19 patients who succumbed to the disease, in the state, according to Mr. Prasad were also having co-morbidities, which refer to the presence of one or more additional physiological or psychological conditions like hypertension and diabetes.
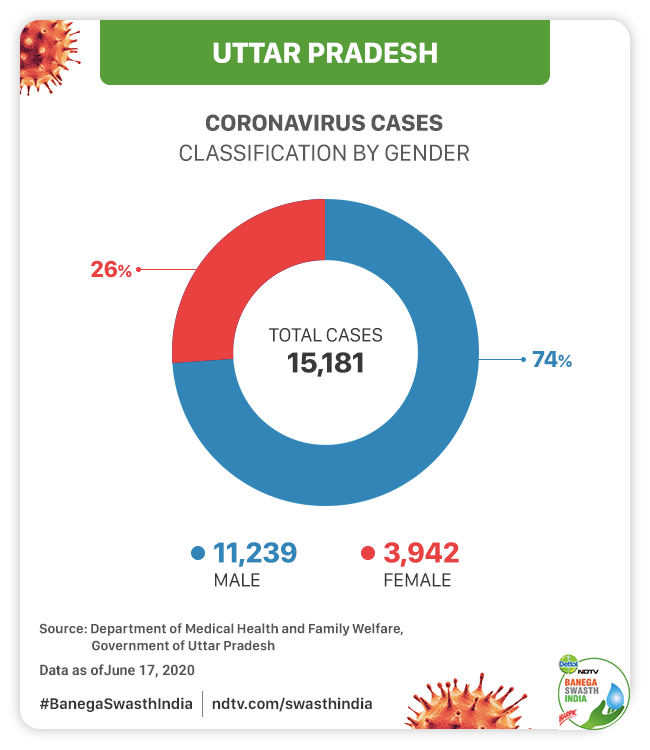
The data on COVID-19 patients provided by the state’s health department shows that men are most affected by the infection. The total number of males tested positive in the state as on June 17 were 11,239 which is almost 74.03 per cent of the total number of cases. Number of females was 3,942 which is approximately 25.97 per cent of the total cases.
Also Read: In Uttar Pradesh’s Firozabad, Violating Coronavirus Guidelines Can Land You In A ‘Mask Ki Class’
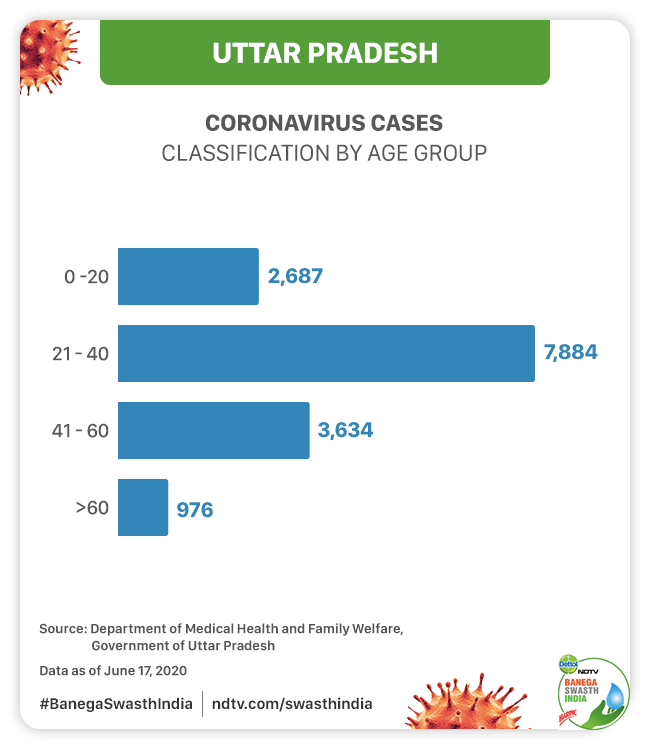
The age-wise data of COVID-19 patients provided by the state shows that the maximum number of cases (7,884) are among the youth in the age group 21-40 years. About 2,687 cases are children in the age group 0-20 years, 3,634 cases are between the age 41-60 years and 976 cases are citizens who are above 60 years of age.
While all 75 districts of the state are affected by the COVID-19 pandemic, the district in the western region of the state especially Agra (1,136, as on June 20) along with district in the national capital region (NCR) like Gautam Budh Nagar (1,369), Ghaziabad (818), Meerut (786) and Bulandshahr (488) are worst-hit. These 5 districts comprise more than one-third of confirmed COVID-19 cases in UP. Agra was the first hotspot of the state and continues to be among the top five districts with the highest number of cases. Dr. Preeti Kumar, Vice President- Public Health System Support at the Public Health Foundation of India said,
The state government has been responsive and particularly focusing on western districts where the cases are high, particularly Ghaziabad, Noida and Meerut. The entire strategy of testing, treating, isolation and quarantine is more intense in these areas. As for Agra, the city did have spikes in May, but now the new cases are low, around 8-10 per day, showing good containment measures; better still, the cure rate is 84 per cent. Sample positivity is around 5.8 per cent, better than the national average. So the city is coping well at the moment; it can further improve testing and maintain vigilance by strengthening surveillance.
From Less Than 100 Tests Per Day In March To Over 18,000 Tests Per Day In June, UP Has Ramped Up Testing
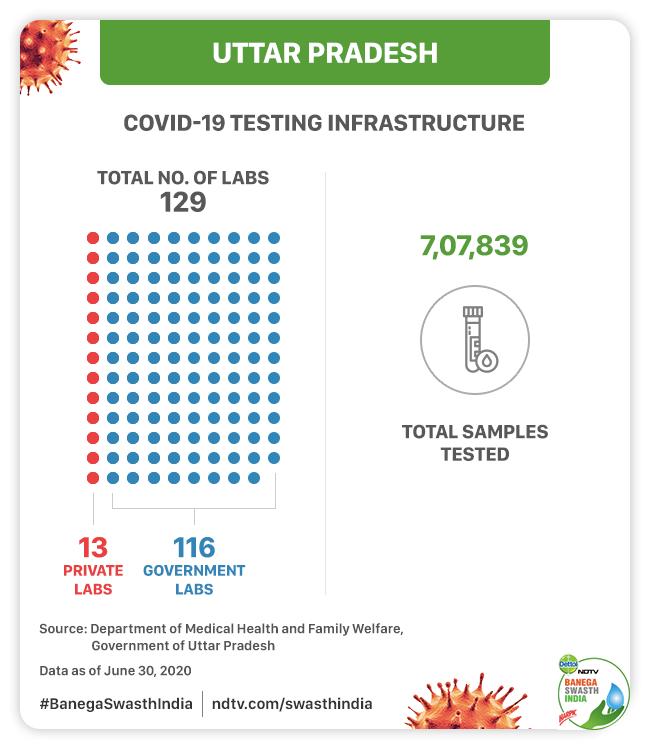
According to Mr. Prasad, when the first case of COVID0-19 was reported in the state in March, there was no testing facility within the state and sample was sent to the National Institute of Virology (NIV), Pune. King George Medical University, Lucknow was the first hospital to get approved for COVID-19 testing and as on June 20, the state has 116 government laboratories and 13 private laboratories that are testing for coronavirus.
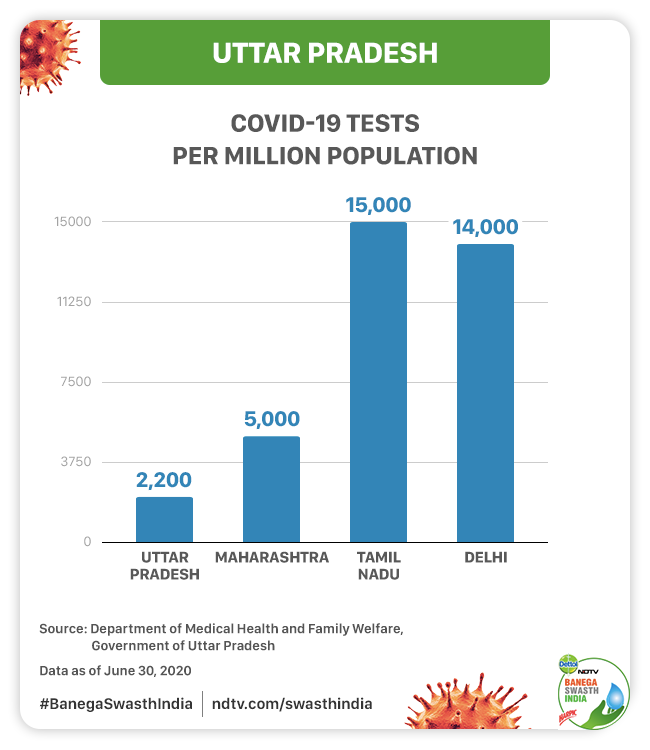
According to Mr. Prasad, earlier in March, the state was testing less than 100 samples per day but over the past three months, the testing capacity has been ramped up to more than 20,000 samples per day. As of June 30, the state has tested more than 7 lakh samples (7,07,839). This accounts to over 2,200 tests per million people, according to the Department of Medical, Health and Family Welfare which is less than the Maharashtra that has done over 5,000 tests per million, Tamil Nadu with over 15,000 tests per million and Delhi that has tested over 14,000 per million population.
The state has been charging no money for tests done in government facilities and a cap of Rs. 2500 per test has been put on testing in private facilities which was Rs. 4,500 earlier. On availability of testing kits and infrastructure, Mr. Prasad said,
We have enough testing kits and conducting testing as per the guidelines of the government. The testing kits can be sourced as and when required. We are facing no challenges on this front.
Also Read: Uttar Pradesh Government Orders Lockdown On Every Weekend Amidst COVID-19 Spread
Uttar Pradesh’s Health Infrastructure
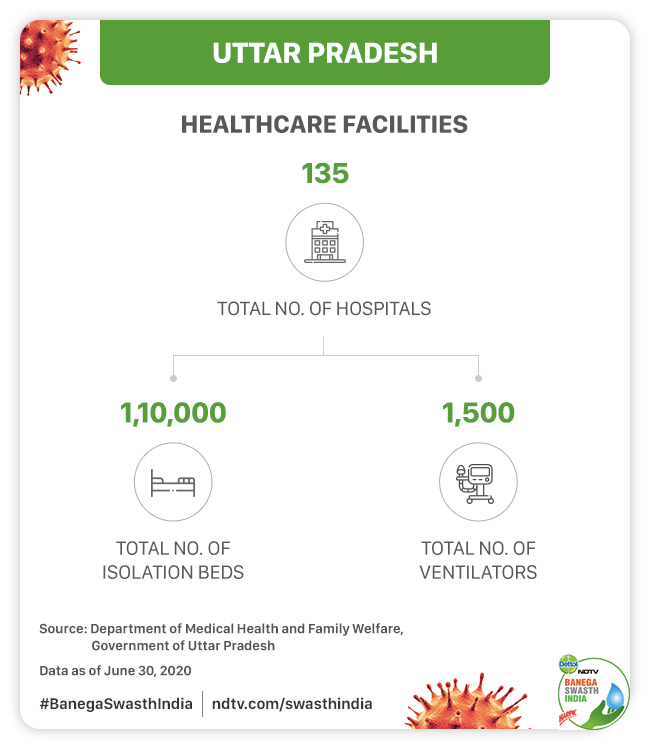
According to Uttar Pradesh’s Health Department, as of now, there are 135 hospitals treating COVID-19. While talking about the adequacy of health infrastructure in UP for fighting the pandemic, Mr. Prasad said that Uttar Pradesh’s Health Department has been able to ramp up the infrastructure significantly over the past three and a half months. The Principal Secretary said,
We have arranged more than 1.1 lakh beds in 75 districts of Uttar Pradesh for COVID-19 patients. Testing, treating, isolation and quarantine is the standard strategy we have adopted which has been prescribed by the government. Currently, we have not been encouraging home isolation and we isolate every COVID-19 positive person in an institutional facility even if somebody is asymptomatic so that they do not infect others.
He further said that the state has dedicated 1,500 ventilators for COVID-19 patients. He said,
Till now, in our experience, only 10-20 patients require ventilators at a time but we have dedicated 1,500 ventilators for COVID-19.
According to Dr. Charan Singh Verma, Associate Professor and Coordinator of Public Health Research, Giri Institute of Development Studies, UP is one such state where health infrastructure is inadequate to meet the demand for health services in the state. Dr. Verma said,
Health is a state subject but during a pandemic crisis like this one, it is very important that the central government step in and support state government. This has been missing and the support seems to be limited to only ‘guidelines making’. Many states are lacking this support including Uttar Pradesh.
Dr. Verma further highlighted that 40 per cent of posts for healthcare staff in the state is still vacant. The National Health Profile, 2019 reveals that the population to doctor ratio in Uttar Pradesh was 2,925 persons covered by one doctor in 2017 which is a huge gap when compared to the WHO (World Health Organisation) recommended doctor to population ratio of 1:1,000.
On the sufficiency of the number of doctors and other healthcare staff present for treating COVID-19 patients, Mr. Prasad said,
We have enough doctors for catering to the current infection load we have in the state. But we have still planned ahead and discussed with the IMA (Indian Medical Association) and other organisation to help us with doctors and medical staff as and when required.
According to an official from the Department of Medical Health and Family Welfare, while the state has been focusing on combating COVID-19, it is ensuring that non-COVID patients are not deprived of treatment. He said,
As far as non-COVID patients are concerned, general OPDs have been started in all Primary Health Centres and Community Health Centres with all necessary COVID-related precautions. Permissions have already been given for conducting surgeries and providing emergency and essential services in all district hospitals. We have trained all doctors and nurses in government as well as private hospitals on infection prevention protocols in order to keep non-COVID patients safe. Each district has a committee that monitors frequently if the protocols are being followed by hospitals or not.
Also Read: Ghaziabad Duo Design App To Match Plasma Donors For COVID Patients
Maternal And Child Care Challenges In The State During The Lockdown
According to UP’s Principal Secretary- Health, because of the unprecedented situations that came with the pandemic, the delivery of services like health, education, nutrition, vaccination and others especially in the rural areas came to the halt in the month of April. However, since the month of May, rural healthcare and nutrition services have started again. Mr. Prasad said,
We have recommenced all our nutrition and immunisation programmes since last month. Our immunisation programme is running every Wednesday and Saturday and all Village Health and Nutrition Day (VHND) programmes are running in every village.
Dr. Kumar highlighted that during the ongoing pandemic, women and children are particularly vulnerable. She said,
Women need more attention during pregnancy in terms of nutrition and addressing deficiencies because the health of women directly affects the health and future of the child. SOPs (Standard Operating Procedures) for management of pregnancies at both public and private facilities, during the ongoing pandemic, are needed.
When NDTV reached out to local activists and frontline workers in various parts of the state, it has found that the nutrition and other rural healthcare services which were completely halted in March and April have indeed slowly started to come back on track. Anita Devi, 40-year-old ASHA in Moradabad district said,
Since May second week, we have been getting iron and calcium tablets for distributing among the pregnant women. We are also conducting immunisation drive every Wednesday and Saturday. We go to each house to tell them that the camp has been set up and then parents bring their children to the camp for vaccination. Maintaining social distancing gets difficult sometimes in villages but we try that there is at least one hand distance among people and their faces are covered with a mask or a scarf. The problem we are currently facing is that we do not get any masks or hand sanitisers from the government to protect ourselves and which scares us a lot because a few of my colleagues have got infected with the coronavirus.
Delivering Healthcare, A Risky Feat For Community Frontline Workers
In UP, the ASHAs (Accredited Social Health Activist) and ANMs (Auxiliary Nurse Midwives) have taken up the crucial work of monitoring the migrant workers who have returned to the state. They go door-to-door enquiring if the household has a returnee and check their symptoms. They also monitor the migrant workers at the quarantine centres. Acknowledging the role and hard work of frontline health workers like Mr. Prasad said,
ASHA workers are tracking migrants who have returned to the state and have reached out to over 18 lakh of them.
In a bid to encourage and honour them, the state government had announced an additional incentive of Rs. 1,000 per month for six months (Jan-June, 2020) for the ASHA workers for participating in combating COVID-19, using National Health Mission fund.
However, when NDTV reached out to AHSAs and ANMs in some parts of UP, it was found that these frontline healthcare workers who are largely women are taking a major life risk in order to perform their duties as they are not being provided with personal protection equipment (PPE) kits, masks, hand sanitisers and other equipment to help them work safely.
While talking about the work done by frontline health workers during the ongoing pandemics, Shashi Singh, 48-year-old Head ASHA at Garwar village in the district of Balia said,
There are more than 1,000 household in this village and five ASHA workers which means that each ASHA worker covers 200 households and at least 4-6 members in one household. So on an average, there are at least 800 people covered by one ASHA worker. We have been constantly conducting door-to-door surveys to identify people with COVID symptoms since the starting of the pandemic. We visit at least 10-12 houses per day. Apart from checking for symptoms, we also raise awareness about coronavirus and have been monitoring the migrant workers also where we get information from.
She added that while they are performing their duties, they are not provided with necessary protective gears to keep themselves from catching the virus. Ms Singh further said,
It was only a month back when we protested that we were given some masks a 100 ml bottle of hand sanitiser. Nothing before that and after. We feel like we are invisible to the state authorities because we are not government employees. Even the Rs. 1,000 incentive that we were promised has not been given to us for the past two months. It is true, I am scared to step out of the house but then what can I do? I live in anxiety every day that I may infect my family.
Gayatri Devi, 42-year-old ASHA worker in Moradabad who has been tested COVID-19 positive is undergoing treatment at a public hospital. While speaking to NDTV she said,
When the entire nation was locked in their houses, we were there out there trying to identify patients by going door-to-door and bring them to Primary Health Centres (PHCs). I did not have any medical mask for any other safety gear. I used to cover my face with a ‘dupatta’. A few days back I got a fever and the next day I got myself tested. When the result came, I was shattered to see that I was positive. My 20-year-old son has got the infection too. We both are fighting this disease now. I am thankful that my other family members are safe.
On the hardships being faced by the frontline workers in UP, Dr. Verma said,
It is a matter of shame that state’s own health workforce was not provided with tools to protect themselves properly. This may be due to lack of funds.
Efforts Taken To Address The COVID-19 Situation In The State
According to Dr. Preeti Kumar, the state government had started acting soon after the first case was reported. She said that with the population as large as UP’s, the state has been able to delay the spike in cases and fatalities because of timely actions. Even before the nationwide lockdown was announced, UP government ordered for shutting down schools, colleges and multiplexes on March 17 and on-going examinations were postponed. On March 22, the Chief Minister announced lockdown of 15 districts. Measures including checks at railway stations and airports, sealing of the borders soon followed. The government has also established helplines for the public (1070). In a bid to ensure that people follow the safety protocols, the state government took strict actions like imposing fines on people for not wearing masks and not following social distancing.
Measures Undertaken By The State To Provide Relief To The Poor
According to the Government of Uttar Pradesh, there are currently 3,962 community kitchens running across the state that are catering to over 3.57 lakh beneficiaries. Apart from this, families of 1.65 crore Antyodaya Anna Yojana workers, workers bearing Mahatma Gandhi National Rural Employment Guarantee Act (MGNREGA) cards as well as construction workers and small wage earners were given one month’s stock of free food grains. Old-Age, Disability and Widow Pension have been paid for two months to 83 lakh beneficiaries.
Amit Tiwari, founder of Uttishtha Foundation, a non-governmental organisation based in Sitapur district that has been distributing cooked meals and ration to the families of daily wage earners who have lost jobs during the lockdown said to NDTV,
The government is providing the ration to those who are cardholders but the truth is that it is not enough. We cannot expect a family to survive on 5 kg rice, 5 kg wheat and 1 kg lentils for one full month and because there is no money to buy from the market, the people are facing a hard time. They don’t have money to buy vegetables, oil, and other ingredients. We are trying to support as much as we can but we also have limited resources. I don’t want to blame the government but I would like to highlight that the intermediaries of the government who are implementing the Public Distribution System must have some level of accountability. Also, there is a high level of confusion as to who is eligible of ration card and who is not because right now, it has been more than three months for many people to have lost the little source of income they had. They have also been pushed below poverty now. They should be eligible for a ration card. As of now, those who do not have ration card are being provided with cooked meals by the government through community kitchen but this is not a sustainable solution because a lot of time these kitchens and food distribution points are far from people.
While sharing his on-ground experience of interacting with the migrant workers who were put into institutional quarantine centres, Mr. Tiwari said,
UP has received a large number of migrants from Delhi, Gujarat and Maharashtra. Ideally, these states should have provided enough food and shelter security to the daily wage workers that they were not forced to become desperate to move back to their villages. It was the responsibility of these states to hold them back and help them stay protected. The migrant influx has further increased the risk of infection and starvation in the state. We can clearly see that the daily wage earners, which form a big proportion of urban poor, were nowhere in the COVID-19 response plan designed at the central and state levels. A lot of the migrant workers have been tested positive. This is how COVID-19 which was earlier urban-centric has reached the villages as well.
On March 28, the UP government deployed 1000 UPSRTC (Uttar Pradesh State Road Tranport Corporation) buses to ferry migrant workers to their native districts during the nationwide lockdown. According to the state government, more than 30 lakh migrant labourers have returned UP following the lockdown.
Over the past three months, the state has built more than 19,000 (19,337) shelter homes/quarantines camps for migrant workers from other states and homeless, across all districts, with provisions for beddings, adequate food, drinking water, cleaning facilities and toilets. Till now, more than 15.96 lakh people have been admitted in these facilities and more than 10,000 people are currently staying in these facilities.
CM Yogi Adityanath announced in March that Rs.1,000 would be given to all daily wage labourers affected due to coronavirus in the state. The state has also created jobs for the migrants and those who lost livelihood in the state under MGNREGA. The state has also launched Atma Nirbhar Uttar Pradesh Rojgar Abhiyan with an aim to provide employment to 1.25 crore migrant workers and cover 31 districts of the state. While acknowledging the state government’s efforts towards creating livelihoods, Dr. Verma said,
See, the state as of now does not have any other option. MGNREGA is the only scheme under which jobs can be created quickly. MGNREGA can provide jobs to a large number of people at the lowest cost. The scheme also provides a legal guarantee of 100 days of work.
The COVID-19 pandemic in Uttar Pradesh, which is also facing a migrant workers crisis shows no slowing down. The state government officials, however, are certain that the state is not facing community transmission yet. The state has utilised the lockdown period for augmenting the health infrastructure. From no testing labs in March to 129 labs in June, the state’s containment strategy includes ‘Test, Trace, Treat’ which has helped the state in achieving a recovery rate higher than the national average. However, the new hotspots cropping up in several districts of the state, especially in the western region is a matter of concern for the state authorities in the fight against COVDI-19.
Also Read: Electronic Care Support Network In Uttar Pradesh To Help Hospitals Treating COVID-19 Patients
NDTV – Dettol Banega Swasth India campaign is an extension of the five-year-old Banega Swachh India initiative helmed by Campaign Ambassador Amitabh Bachchan. It aims to spread awareness about critical health issues facing the country. In wake of the current COVID-19 pandemic, the need for WASH (Water, Sanitation and Hygiene) is reaffirmed as handwashing is one of the ways to prevent Coronavirus infection and other diseases. The campaign highlights the importance of nutrition and healthcare for women and children to prevent maternal and child mortality, fight malnutrition, stunting, wasting, anaemia and disease prevention through vaccines. Importance of programmes like Public Distribution System (PDS), Mid-day Meal Scheme, POSHAN Abhiyan and the role of Aganwadis and ASHA workers are also covered. Only a Swachh or clean India where toilets are used and open defecation free (ODF) status achieved as part of the Swachh Bharat Abhiyan launched by Prime Minister Narendra Modi in 2014, can eradicate diseases like diahorrea and become a Swasth or healthy India. The campaign will continue to cover issues like air pollution, waste management, plastic ban, manual scavenging and sanitation workers and menstrual hygiene.
[corona_data_new]