New Delhi: Malnutrition is a crisis in India and has remained a silent emergency for long. In 2017, malnutrition was responsible for two-thirds of child deaths in India, killing 706,000 children under five. In a bid to change this scenario and fight the deeply rooted malnutrition in the country, the government has started making policy and direct interventions and has also been undertaking various initiatives in collaboration with non-governmental organisations. However, experts say that making concerted efforts is the key to make India a healthy and malnutrition free country.
Also Read: How Nutrition During First 1000 Days And Anaemia In Mothers Is Linked To Malnutrition In Children
Earlier, Prime Minister Narendra Modi issued a pledge that India will become free from malnutrition by 2022. According to the National Nutrition Strategy of 2017, the aim is to achieve a malnutrition-free India by 2022. For this, the plan is to reduce stunting or low-height-for-age prevalence in children (0-3 years) by about three percentage points per year by 2022 from NFHS-4 (National Family and Health Survey-4) levels, and achieve a one-third reduction in anaemia in children, adolescents and women of reproductive age.
According to experts, the problem of malnutrition is inter-generational and is dependent on multiple factors like breastfeeding, Optimal Infant & Young Child Feeding (IYCF) practices, immunization, institutional delivery, food fortification, deworming, dietary diversification, and access to safe drinking water & proper sanitation (WASH).
Malnutrition remains a silent emergency in India but one sees a substantial improvement in health and well-being since the country’s independence in 1947. Dr Ranjan, Tata Trust shared with NDTV about how long a way has India come. He said,
We have made significant progress in reducing malnutrition, but the problem is that the progress that we are making is not enough. You know the rate at which we are making the progress is what is bothersome. With the economic status that India has today and the available resources in terms of nutrition interventions and the infrastructure that we have created, we should be making a far more rapid decline in malnutrition. That is unfortunately not happening.
The POSHAN Abhiyaan, provides an opportunity to counter malnutrition and usher in a new era in food and nutrition security. To address the problem of stunting, under-weight and wasting, especially in children sustained efforts with multi-pronged approach, grass-root synergy and convergence is the key. Vinod Paul, Member, NITI AAYOG speaks about the various policies India has always had but what the POSHAN Abhiyaan aims to do. He said,
Poshan Bhiyan, the national nutrition mission aims to bring in massive acceleration in decline of undernutrition in children and also to address anaemia in children and women both. It brings together food intervention, breast feeding intervention but equally importantly the intervention in health sector which are so very important. It has a focus on first 1000 days of life which means 9 months of pregnancy and first 2 years of child’s life.
In recognition of the remaining challenges in nutrition, health and hygiene/sanitation, besides the POSHAN Abhiyaan (National Nutrition Mission), the Government of India has also launched the National Health Mission and Swachh Bharat Abhiyaan (water, sanitation and hygiene) Mission, and ayushmann Bharat. The government has matched the commitment by creating ambitious targets and supporting efforts with substantial budgets.
Also Read: Malnutrition In India: Has This Decade Laid Down A Blueprint For A Malnutrition-Free India?
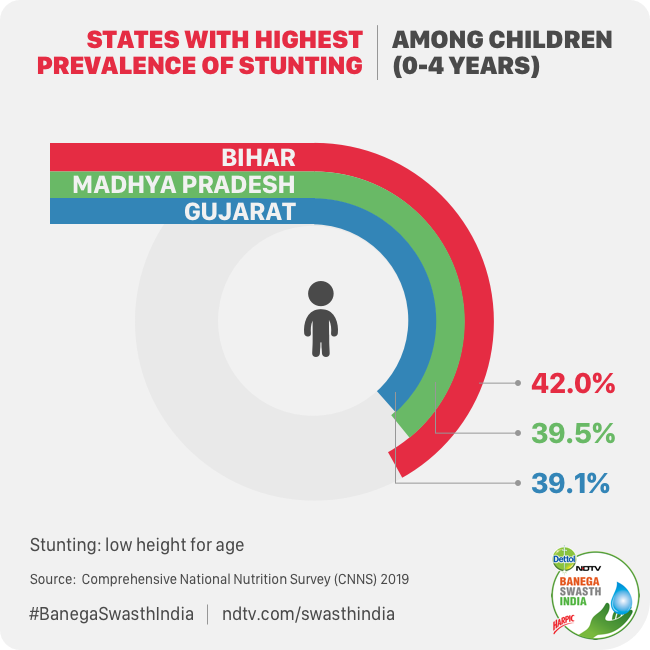
If stunting and underweight affects the rural population, aneamia and double burden of obesity is a huge challenge in the urban setting. Unsurprisingly, the malnutrition burden is far from equally shared between India’s states and union territories. A number of the most populous states like Bihar, Madhya Pradesh, Rajasthan and Gujarat have a high stunting prevalence whereas the lowest prevalence of stunting was found in Goa and erstwhile state of Jammu and Kashmir.
According to the Comprehensive National Nutrition Survey (CNNS) 2019 report a higher prevalence of stunting in under-fives was found in rural areas (37%) compared to urban areas (27%). Also, children in the poorest wealth quintile were more likely to be stunted (49%), as compared to 19% in the richest quintile.
Soumya Swaminathan, Deputy Director General, Programmes, World Health Organization said that it is also important is to understand the differences between the states so if looked at the life expectancy while has been achieved tremendous gains on life expectancy over the last 25 years there is still a ten year difference between Kerala for example and Assam or Uttar Pradesh if mortality under the age of 5 years is taken. She said,
So you know deaths in children under 5 there is a fourfold difference again between the most developed and least developed states. So addressing the risk factors of disease burden in every state is going to be important for local policy and programing. So I think it is important to keep in mind the major disease groups and risk factors that affect every state but also to look at equity issues between states and within states there are groups that have worst health outcomes and worst health parameters than other groups and I think we need to focus our attention on those groups.
Also Read: Here Are Tips On How To Tackle ‘Hidden Hunger’ In Children Caused By Lack Of Micronutrients
The NFHS-4 shows wide inter-state and inter-district variations in the prevalence of all three indicators of undernutrition in the country. It is necessary to identify the specific causes of under-nutrition in each District and provide targeted interventions after identifying the exact cause(s) in those areas. That is the reason Niti Aayog has selected 113 Districts to bring about improvement in nutritional status in a time bound manner along with help of leveraging technology. Dr Vinod Paul, NITI Aayog added,
We looked at how to classify districts with low development indicator and low indicators related to health and nutrition. And stunting rates and as well as infant mortality rate was accounted for. Now as part of the honorable prime minister’s programme on aspirational districts and which the massive emphasis is on health and nutrition. We are providing smart phones to the anganwadi worker, the idea of the smart phones is twofold. One use the phone screen for educational messages, on feeding and how to look after the child. But also the other purpose is to provide monitoring of the children and look at their weight, the data can be transmitted.
Government programmes for Vitamin A supplementation and iron-folic acid (IFA) supplementation for pregnant women and adolescent girls have been in operation for over five decades. Food Fortification which is a process by which vitamins and minerals are added to commonly consumed foods, offers a good opportunity to improve the micronutrient status of people without changing their food habits. Keeping in mind the issue of deficiency of micronutrients, food Fortification helps in adding micronutrients into foods that does not already contain them. Like milk is often fortified with additional vitamin A & D, to boost its nutritional value. The aim of fortification is to help people remedy their nutritional deficiencies. Sangram Chaudhary,Managing Director, Mother Diary Fruit & Vegetable said,
In metros because of the lifestyle children and people are not exposed to sun and Vitamin D deficiency is developed. And in rural areas, malnutrition is a major problem. And it is our collective responsibility that we fortify our food, especially milk because milk is a very good vehicle for carrying these micronutrients. Earlier the fat soluble vitamin a and d were available, now even water soluble vitamin D and A are available. And mother dairy has been the pioneer, thanks to Dr Kurien’s vision. In 1984 when we started the bulk vending system, our milk was fortified with vitamin A and we continue to fortify our bulk vending token milk. Recently we have been fortifying the other variants also, I wish that all the variants can be fortified. FSSAI should allow that all the milk variants can be fortified.
Also Read: Only 9 Per Cent Children Get Nutritious Food: Union Minister Smriti Irani
The Food Fortification Resource Centre has taken the onus of major widespread production of fortified foods, creating a ‘+F’ logo for food the following staple foods: rice, wheat flour, salt, edible oil, and milk.
Pawan Agarwal, FSSAI shared with NDTV that micronutrients, Vitamins A & D, Vitamin B12, Iron, folic acid are essentials and are like magic wand for human body. He further said that they are required in such small quantities but do wonders. He said,
These are required by all of us in sufficient quantities and our food system unfortunately are not providing so. So we are promoting fortified staples wheat flours, rice, double fortified salts, edible oil and milk.
Vaccines also help prevent some of the chronic consequences of malnourishment. Mission Indradhanush aims to reach out to the unreached children and increase the coverage of immunization in the country at a rate of 6-7% annually.
Implementation of any programme is the key for its success so the Swasth Bharat Prerak programme, a joint initiative of the Ministry of Women & Child Development and the Tata Trust supplements the path-breaking POSHAN Abhiyaan by providing managerial and administrative support to the district and state administration for the effective implementation of the mission. Dr Ranjan,Tata Trust added,
Many of these preraks are young graduates, just out of college. They are very enthusiastic about this, they have been given some training. In the last 18 months or so we have had around 500 preraks, each working at the district level. At any given time more than 350 districts are covered, almost 90% of aspirational districts are covered. They are the go between the different departments and just help implement the very well-conceived and planned implementation of frame work of POSHAN abhiyaan.
India is the anemic capital of the world and anemia is the reason for almost 20-40% maternal deaths in our country. Simple steps like eating right like including iron rich food in our diet can help fight these startling numbers. Smile foundations Swabhiman programme aims to impart this knowledge to expecting mothers and adolescent girls and overcome aneamia. Sanju was detected anemic 6 months ago. Her hemoglobin level was 6 mg but with intervention today her hemoglobin is 10.
I take my medicines plus started eating healthy iron rich food like gur channa, palak and feels much more healthier from within.
In the battle to eradicate malnutrition in Maharashtra timely intervention by the nutrition programme in Amravati and Nandurba has ensured that the lives of the poorest…most vulnerable and malnourished children have been saved… Forty one community nutrition workers are already on the ground in Melghat and in some villages they are simply identified by their outfit. Ravi Bhatnagar, RB told NDTV,
Community Nutrition Workers try to find out the households which are at risk. They support the district administration, the state administration. They help in referrals of malnourished kids to the Nutrition Rehabilitation Centre, they educate mothers on the role on nutrition. We have introduced certain game tools like the Poshan Thali. So these women who are the ground with us, they don’t just promote the nutrition part, they also work on the lactation part, which means that they promote breastfeeding on the ground.
Also Read: Nutritional Requirements Of A Baby From 0-2 Years
Sukhmani Bhilawekar is happy that her son now has the energy to play as the baby was born underweight. She said, “My baby was just 1kg during the delivery. We had to go to Amravati and we stayed for one month there. Then we came back here and for three months he would keep crying. He was admitted into the NRC and then slowly he started driking milk.”
Sarita, Community Nutrition Worker shared,
We follow up with the families that do not send their kids to the NRC and we meet families whose kids have returned from the NRC for six months and educate them about the importance of hygiene which we teach them about all this through videos.
The Integrated Child Development Services program was started by the Indian government in 1975 to combat child hunger and malnutrition. Today there are more than 1.3 million Anganwadi centre spread out across India, that deliver early education, health, and nutrition services as part of the country’s Integrated Child Development Services (ICDS) scheme. Perhaps the largest mother and child nutrition and care programme of its kind in the world.
Another initiative is the Mid Day Meal Scheme which aims to improve attendance & retention by providing free food in government & local primary schools but often the quality of food is compromised.
Though we have health care programmes and policies but what are the missing linkages?? Or is implementation a cause for concern… There are many success stories of various state Govt’s that can also be replicated across the country. Basanta Karr, an expert on nutrition said,
There are many gold impact models in India. So there are many states have shown tremendous results. So if some states in India have shown anemia reduction, if some states have shown stunting or underweight reduction. If you put our efforts and best practices together, why not India cannot achieve.
To achieve malnutrition-free status, India’s development agenda needs to tackle its ‘double burden’ of malnutrition—under-nutrition and obesity at the same time. The Poshan abhiyaan needs to become a jan andolan (people’s movement) people need to be aware about nutrition, making the correct diet choice. It is important that as citizens we take responsibility along with all stakeholders for a truly healthy India.